Updated: May 2024
Published: March 2020
Fully referenced facts about covid, provided by experts in the field, to help our readers make a realistic risk assessment. (Regular updates below).
“The only means to fight the plague is honesty.” (Albert Camus, 1947)
Overview
- Lethality: The overall infection fatality rate (IFR) of the novel coronavirus in the general population (excluding nursing homes) is about 0.1% to 0.5% in most countries, which is most closely comparable to the medium influenza pandemics of 1936, 1957 and 1968.
- Age profile: The median age of covid deaths is over 80 years in most Western countries (78 in the United States) and about 5% of the deceased had no medical preconditions. In many Western countries, about 50% of all covid deaths occurred in nursing homes.
- Vaccine protection: Covid vaccines provided a high but rapidly declining protection against severe disease. Vaccination could not prevent infection and transmission (known since June 2021). A prior infection conferred a more durable immunity than vaccination.
- Vaccine injuries: Covid vaccines caused severe and fatal vaccine reactions, including cardiovascular, neurological and immunological reactions. Because of this, the risk-benefit ratio of covid vaccination in healthy children and adults under 50 years of age was poor.
- Excess mortality: Global pandemic excess mortality is close to 20 million deaths, which is about 15% compared to normal global mortality and about 0.25% compared to global population. Some of the additional deaths were caused by indirect effects of the pandemic and lockdowns.
- Symptoms: About 30% of all infected persons show no symptoms. Overall, about 95% of all people develop at most mild or moderate symptoms and do not require hospitalization. Age and obesity, in particular, are major risk factors for severe covid.
- Treatment: For people at high risk or high exposure, early or prophylactic treatment is essential to prevent progression of the disease. Numerous studies found that early outpatient treatment of covid can significantly reduce hospitalizations and deaths.
- Long covid: Up to 10% of symptomatic people experience post-acute or long covid, i.e. covid-related symptoms that last several weeks or months. Long covid may also affect young and previously healthy people whose acute covid infection was rather mild.
- Transmission: Indoor aerosols appear to be the main route of transmission of the coronavirus, while outdoor aerosols, droplets, as well as most object surfaces appear to play a minor role. Pre-symptomatic transmission may account for about 30% of all community infections.
- Masks: Face masks had no influence on infection rates, which was already known from studies prior to the pandemic. Even N95 masks had no influence on infection rates in the general population. Moreover, long-term or improper use of face masks can lead to health issues.
- Lockdowns: In contrast to early border controls (e.g. by Australia), lockdowns had no significant effect on the pandemic. However, according to the World Bank lockdowns caused an “historically unprecedented increase in global poverty” of close to 100 million people.
- Children and schools: In contrast to influenza, the risk of severe covid in children is rather low. Moreover, children were not drivers of the pandemic and the closure of schools had no effect on infection rates in the general population.
- PCR tests: The highly sensitive PCR tests are prone to producing false positive or false negative results (e.g. after an acute infection). Overall, PCR and antigen mass testing had no effect on infection rates in the general population (exception: to sustain border controls).
- Contact tracing: Manual contact tracing and contact tracing apps on mobile phones had no effect on infection rates. Already in 2019, a WHO study on influenza pandemics concluded that contact tracing is “not recommended in any circumstances”.
- Vaccine passports: Vaccine passports had no effect on infection rates as vaccination cannot prevent infection. Vaccine passports could, however, serve as a basis for the introduction of digital biometric identity and payment systems. NSA whistleblower Edward Snowden warned already in March 2020 that surveillance could be expanded during the pandemic.
- Virus mutations: Similar to influenza viruses, mutations occur frequently in coronaviruses. The omicron variant, which may have emerged from vaccine research, showed significantly higher infectiousness and immune escape, but 80% lower lethality.
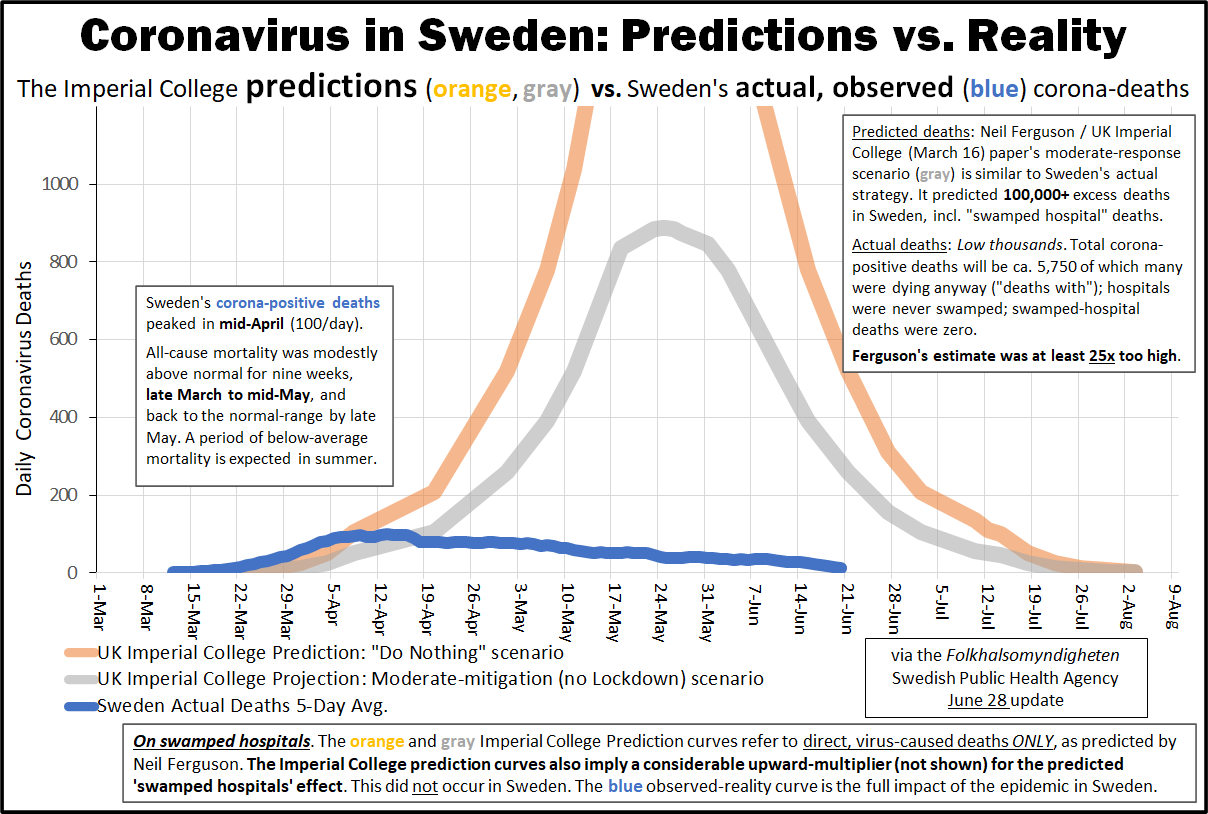
- Sweden: In Sweden, covid mortality without lockdown was comparable to a strong influenza season and somewhat below the EU average. About 50% of Swedish deaths occurred in nursing homes and the median age of Swedish covid deaths was about 84 years.
- Influenza viruses: Influenza viruses largely disappeared during the coronavirus pandemic. This was not a result of “covid measures”, but a result of temporary displacement by the novel coronavirus, even in countries without measures (such as Sweden).
- Media: Overall, media reporting on the pandemic was rather unprofessional, increased fear and panic in the population and caused a hundredfold overestimation of covid lethality. Some media outlets even used manipulative pictures and videos to dramatize the situation.
- Virus origin: Genetic evidence points to a laboratory origin of the new coronavirus. Both the Virological Institute in Wuhan (WIV) as well as some US laboratories that cooperated with the WIV performed various kinds of research on similar coronaviruses.
Latest Articles
General
- Why the smartest people failed (July 2023)
- The Nine Great Covid Mysteries (June 2022)
- Why Covid is a Strange Pandemic (Sept. 2020)
- Global Excess Mortality Update (December 2023)
Earliest Articles
- A Swiss Doctor on Covid-19 (March 14, 2020)
- Corona, the Media, and Propaganda (March 19, 2020)
- Open Letter from Professor Sucharit Bhakdi (March 28, 2020)
Media and Propaganda
- Pandemics and Propaganda (December 2022)
- The Propaganda Pandemic (February 2022)
- Covid and Reality (September 2022)
- Covid and Culture (December 2023)
Coronavirus Origins
- On the Origins of SARS-CoV-2 (June 2020)
- Did China stage the Wuhan videos? (April 2021)
- Omicron hits the mutation jackpot (November 2021)
Lockdowns
- The Lockdown Lunacy in Retrospect (March 2023)
- Open letter by Prof. Ehud Qimron (January 2022)
- Judgment Day: Sweden Vindicated (December 2021)
- Sweden: The Battle over Pandemic Reality (May 2023)
Covid Vaccines (General)
- Covid Vaccines: Facts, Fears, Fraud (March 2023)
- Covid Vaccines: A Reality Check (December 2022)
- How effective are covid vaccines, really? (June 2022)
- Covid Vaccines: Vaccines or Gene Therapy? (Dec. 2021)
- The Power of Natural Immunity (December 2021)
- Covid Vaccines: Hope or Hype? (November 2020)
Vaccine Adverse Events
- DNA contamination in mRNA vaccines (Nov. 2023)
- Covid Vaccines and Fertility (March 2023)
- Covid Vaccine Adverse Events (June 2021)
Vaccine Passports
- From “Vaccine Passports” to Digital Identity (May 2023)
- Israel: Highest Infection Rate in the World (Sept. 2021)
- The failure of “vaccine passports” (July 2021)
- The “Vaccine Passport” Agenda (February 2021)
- The WEF and the Pandemic (October 2021)
Face masks
- The Face Mask Folly in Retrospect (August 2021)
- WHO Mask Study Seriously Flawed (September 2020)
- Are Face Masks Effective? The Evidence (July 2020)
PCR Testing
- The trouble with PCR tests (October 2020)
- The failure of PCR mass testing (June 2021)
- The “zero covid” countries (December 2020)
Early Treatment
- Covid treatments in retrospect (May 2024)
- On the Treatment of Covid-19 (July 2020)
- Severe covid and auto-immunity (July 2021)
- The Ivermectin Debate (July 2021)
Coronavirus Disease
- Studies on Covid-19 Lethality (May 2020)
- Post-Acute Covid and Long Covid (August 2020)
- Covid and Kids: The Evidence (February 2021)
- Obesity and the Pandemic (June 2021)
- Coronavirus doesn’t exist? (April 2022)
Covid and the flu
- Why the flu has disappeared (February 2021)
- The return of the flu (November 2021)
- Covid vs. the flu, revisited (March 2021)
Coronavirus Transmission
- Pre-symptomatic transmission (June 2021)
- What about a Third Wave? (February 2021)
- Covid: Just A “Casedemic”? (August 2020)
Videos
- Coronavirus Pandemic (SPR Media Archive)
Chart