Updated: June 2021
Published: October 2020
How useful are population-wide PCR coronavirus tests?
Back in March 2020, SPR explained that the highly sensitive PCR tests are prone to producing clinically misleading results and that their individual predictive value may easily drop below 50%.
The issues with PCR tests are numerous:
- There can be large-scale test kit contamination, as both the US and the UK (and several African countries) discovered during the early phase of the pandemic.
- There can be testing site or lab contamination, which has led to countless false positive results, school closures, nursing home quarantines, canceled sports events, and more.
- The PCR test can react to other coronaviruses. According to lab examinations, this happens in about 1% to 3% of cases if only one target gene is tested, as is the case in many (but not all) labs and as the WHO itself has recommended to avoid ambiguous positive/negative test results.
- The PCR test can detect non-infectious virus fragments weeks after an active infection, or from an infection of a contact person, as the US CDC confirmed.
- The PCR test can detect viable virus in quantities too small to be infectious (see below).
If the virus is not widespread in a population, and there is no test kit or lab contamination, and labs test for at least two target genes, the risk of a false-positive result is low. This is why, for instance, New Zealand at times had no positive PCR tests for weeks despite frequent testing.
But if there is an ongoing infection wave, or if there has been a recent infection wave, or if labs test only for one gene sequence or struggle with contamination, things get more complicated.
A PCR test is amplifying samples through repetitive cycles. The lower the virus concentration in the sample, the more cycles are needed to achieve a positive result. Many US labs work with 35 to 45 cycles, while many European labs work with 30 to 40 cycles.
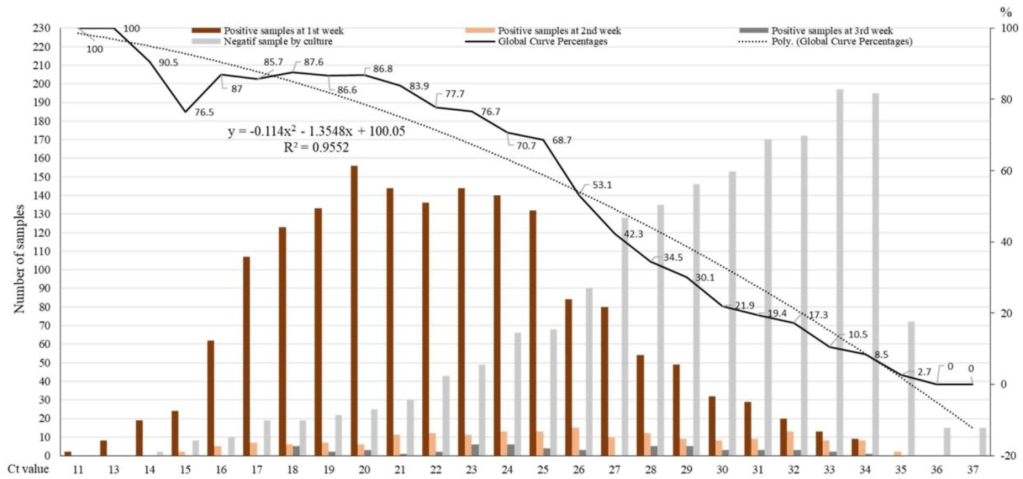
The research group of French professor Didier Raoult has recently shown that at a cycle threshold (ct) of 25, about 70% of samples remained positive in cell culture (i.e. were infectious); at a ct of 30, 20% of samples remained positive; at a ct of 35, 3% of samples remained positive; and at a ct above 35, no sample remained positive (infectious) in cell culture (see diagram).
This means that if a person gets a “positive” PCR test result at a cycle threshold of 35 or higher (as applied in most US labs and many European labs), the chance that the person is infectious is less than 3%. The chance that the person received a “false positive” result is 97% or higher.
(Note that the exact figures depend on the test and lab in question, and that if a sample was already positive at a lower cycle threshold (e.g. 20), chances of infectiousness are much higher.)
Juliet Morrison, a virologist at the University of California, Riverside, explained to the New York Times: “Any test with a cycle threshold above 35 is too sensitive. I’m shocked that people would think that 40 could represent a positive. A more reasonable cutoff would be 30 to 35.” According to the New York Times, up to 90% of positive tests at a cycle threshold of 40 would be negative at a ct of 30.
Why do labs use such high ct values? From a lab perspective, it is safer to produce a “false positive” result that puts a healthy, non-infectious person into quarantine, than to produce a “false negative” result and be responsible if someone infects their grandmother.
However, a negative result at a cycle threshold above 35 still does not exclude a covid infection, as a false negative result may arise if the sample is taken improperly or too early. More recently, US researchers found that single-gene tests were false-negative due to new virus mutations.
The above considerations are valid at the individual level. At the aggregate level, if the adjusted number of positive PCR tests is suddenly increasing, this certainly indicates an infection wave. The problem then is that in many places, PCR testing has been catching at most 10% of all infections.
In conclusion, while PCR tests at high-risk places like hospitals, nursing homes and other sensitive locations are vital and undisputed, the benefit of mass PCR testing in the general population, which is costing mid-sized countries billions of dollars, may be somewhat more debatable.
Update I: In January 2021, the WHO fully confirmed the above analysis: “WHO guidance ‘Diagnostic testing for SARS-CoV-2’ states that careful interpretation of weak positive results is needed. The cycle threshold (Ct) needed to detect virus is inversely proportional to the patient’s viral load. Where test results do not correspond with the clinical presentation, a new specimen should be taken and retested using the same or different () technology. WHO reminds (PCR test) users that disease prevalence alters the predictive value of test results; as disease prevalence decreases, the risk of false positive increases.” (WHO Information Notice for IVD Users 2020/05)
Update II: The failure of PCR mass testing (June 2021)
You have been reading: The Trouble with PCR Tests.
An analysis by Swiss Policy Research.
