Publiziert: 17. Februar 2022 (akt.)
Teilen auf: TW / FB / TG
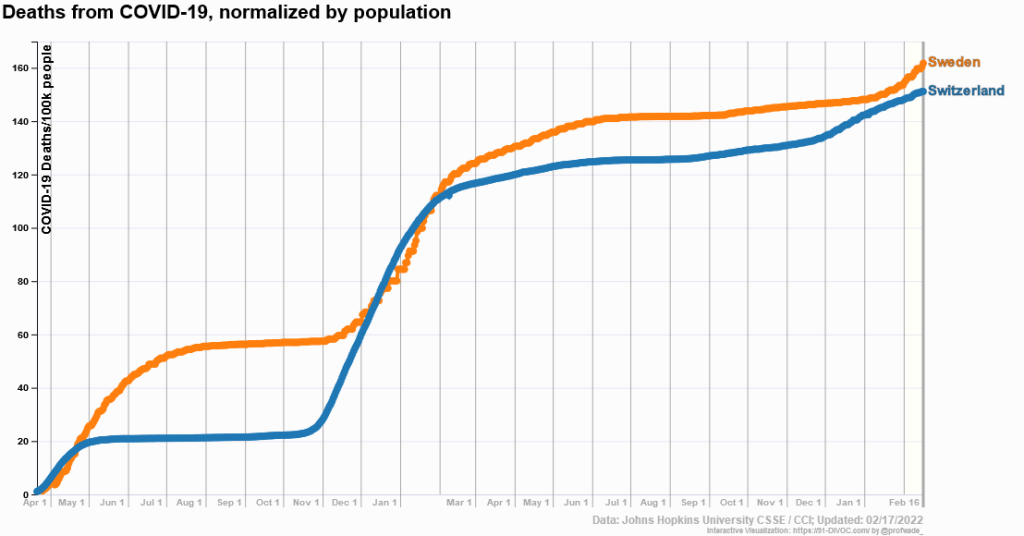
Die Schweiz hat die meisten “Corona-Maßnahmen” aufgehoben. Doch der Vergleich mit Schweden zeigt: Außer sozialen und ökonomischen Schäden haben sie nichts gebracht.
Hinweis: Bei Sprachfehlern die automatische Seitenübersetzung deaktivieren.
Schweiz versus Schweden
Die Schweiz hat während der Corona-Pandemie im internationalen Vergleich eine der am wenigsten restriktiven Strategien gewählt. Dennoch entschied sich die Schweiz im Unterschied zum liberalen Schweden für verschiedene Corona-Maßnahmen, darunter insbesondere ein teilweiser Lockdown im Frühjahr 2020 und Winter 2020/2021, Schulschließungen im Frühjahr 2020, eine Maskenpflicht insbesondere im öffentlichen Verkehr und Einzelhandel sowie teilweise in Schulen, Massentests und ausgebaute Kontaktverfolgung, sowie schließlich “Covid-Zertifikate”.
Haben sich diese Maßnahmen und Einschränkungen für die Schweiz gelohnt? Der von Politik und Medien gefürchtete Vergleich mit Schweden zeigt: Die Schweizer Maßnahmen haben keinen erkennbaren Vorteil gebracht. Während die Schweiz bei den reinen Corona-Todesfällen (siehe Grafik oben) ganz leicht unter Schweden liegt (1.5 vs. 1.6 Todesfälle pro 1000 Einwohner), liegt die Schweiz bei der Übersterblichkeit sogar leicht über Schweden (1.4 vs. 1.1 Todesfälle pro 1000 Einwohner).
Die Schweiz und Schweden sind dabei demographisch sehr gut vergleichbar: ähnliche Bevölkerungsgröße (8.7 vs. 10.5 Millionen), Lebenserwartung (83.4 vs. 82.4), Anteil Einzelhaushalte (38% vs. 40%), Adipositas-Rate (20% beide), Impfrate (68% vs. 74%), und gewichtete Bevölkerungsdichte (3000 vs. 2700; zum Vergleich Norwegen 900 und Finnland 985).
Auch internationale Studien haben inzwischen gezeigt, dass Lockdowns, Masken, Schulschließungen, Massentests und Kontaktverfolgung sowie die “Covid-Zertifikate” keinen Einfluss auf die Pandemie und die Corona-Mortalität hatten. Einen deutlichen Effekt hatten einzig frühzeitige und permanente Grenzschließungen in Ländern wie Island, Australien und Neuseeland, was für die Schweiz indes keine realistische Option war (mehr dazu gleich).
Eine detaillierte Analyse zeigt, dass der Altersmedian der Schweizer Corona-Todesfälle bei etwa 84 Jahren lag und sich etwa 50% davon in Altersheimen ereigneten. Bei Personen unter 65 Jahren lag die Sterblichkeit in den Jahren 2020 und 2021 jeweils im Rahmen einer starken saisonalen Grippewelle (wie 2015), bei Personen über 65 lag sie 2021 dank der Impfung ebenfalls im Rahmen einer Grippewelle, im Winter 2020/2021 jedoch noch deutlich darüber (siehe Grafiken unten).
Insgesamt lässt sich sagen, dass die Virulenz des neuen Coronavirus einem typischen Grippevirus entspricht, ähnlich der Asiatischen Grippe von 1957 oder der Hongkong-Grippe von 1968 (als zugleich das Woodstock-Festival stattfand), aber weit milder als die “Spanische Grippe” von 1918; allerdings traf das Coronavirus auf eine deutlich ältere Bevölkerung mit diversen metabolischen Vorerkrankungen und vor allem ohne spezifisches Immungedächtnis – im Unterschied zu den Grippe-Pandemien, bei denen Menschen über 50 zuvor bereits Kontakt mit ähnlichen Viren hatten.
Während Schweden mit minimalen Einschränkungen durch die Pandemie kam und in einem umfassenden ökonomischen Ranking des britischen Economist zuletzt auf dem weltweit dritten Platz landete, waren die diversen Restriktionen für die Schweiz mit hohen sozialen und ökonomischen Schäden verbunden: Die unwirksamen Lockdowns, Masken, Massentests und Kampagnen (1) sowie die wirtschaftlichen Ausfälle und zusätzlichen Sozialleistungen (2) kosteten insgesamt wohl gegen einhundert Milliarden Franken – Geld, das besser in die (Früh-)Behandlung tatsächlicher Corona-Patienten investiert worden wäre; zugleich hat sich die Anzahl der schwer depressiven Menschen in der Schweiz durch die unnötigen Restriktionen mehr als verfünffacht und die Kliniken registrierten einen massiven Anstieg an suizidalen Kindern und Jugendlichen.
Die Weltbank räumte derweil ein, dass Lockdowns, und nicht die Pandemie selbst, zu einer “historisch einzigartigen Zunahme” an weltweiter Armut um knapp 100 Millionen Menschen (!) geführt haben. In Ländern wie Uganda fielen durch Lockdowns und Schulschließungen 50% der Kinder aus dem Bildungssystem und 30% davon dürften aufgrund von “Jugendschwangerschaften, Frühverheiratungen und Kinderarbeit” nicht mehr in die Schule zurückkehren.
Schweden ist überdies ein gutes Beispiel dafür, dass die “Corona-Maßnahmen” selbstverständlich auch nicht zum Verschwinden der Grippe und anderer Viren beigetragen haben, denn tatsächlich verschwanden diese Viren auch in Staaten ohne solche Maßnahmen, wie eben Schweden, Florida, Japan oder Belarus. Der Grund: Sie wurden durch das neue Coronavirus verdrängt und kehrten erst bei einer natürlichen Corona-Immunität von circa 80% wieder zurück, was zuerst in Indien der Fall war. Virale Verdrängung wurde bereits bei den früheren Grippe-Pandemien beobachtet.
Der Tages-Anzeiger (Tamedia) verglich die Schweiz zuletzt noch mit Dänemark, tatsächlich einem der erfolgreichsten Länder Europas während der Pandemie, und wollte seinen Lesern weismachen, die Schweiz hätte mehr Restriktionen benötigt, um erfolgreicher zu sein. Doch das ist Unsinn: Nachbar Österreich hatte eines der strengsten Regime Europas und schnitt dennoch deutlich schlechter ab als die Schweiz. Der Vorteil Dänemarks war die isolierte Lage (ähnlich wie Singapur in Asien) mit zwanzig mal weniger Grenzpendlern als die Schweiz sowie die frühen und konsequenten Grenzschließungen. Die dänische Strategie war für die Schweiz deshalb kaum realistisch.
Das “Covid-Zertifikat”
Der Tiefpunkt der Schweizer Corona-Pandemie war zweifellos die Einführung des sogenannten “Covid-Zertifikats” im September 2021 sowie der teilweise Ausschluss von ungeimpften und ungenesenen Personen vom öffentlichen Leben im Dezember 2021.
Tatsächlich war aufgrund von Daten aus Impfvorreiter Israel bereits seit Juni 2021 bekannt, dass die Impfung Infektionen nicht verhindern kann und dass geimpfte und ungeimpfte Personen gleich ansteckend sind. Seit Spätherbst war die Infektionsrate bei Geimpften sogar höher als bei Ungeimpften, woraufhin das BAG die Erfassung dieser unangenehmen Daten einfach einstellte.
Aus historischer Sicht ist klar, dass die epidemiologisch in keiner Weise gerechtfertigte, biomedizinische Diskriminierung von Schweizer Bürgern zu den dunkelsten Kapiteln der modernen Schweizer Geschichte zu zählen ist, zusammen mit anderen gravierenden Verfehlungen wie den “Verdingkindern”, der Fichen-Affäre, dem Raubgold oder dem Schweizer “Judenstempel”. Dass dabei erneut ein Großteil der Schweizer Bevölkerung mitmachte oder schwieg – wie beim Referendum vom 28. November 2021 sichtbar wurde – wirft kein gutes Licht auf die Schweiz.
Es sei noch einmal daran erinnert, wer die Schweizer in einer beispiellosen Angst- und Propaganda-Kampagne zur Annahme des “Covid-Zertifikats” verführte: Der Schweizer Gesundheitsminister mit spektakulären Falschaussagen (“mit dem Covid-Zertifikat kann man zeigen, dass man nicht ansteckend ist”); der Leiter der Pro-Kampagne, ein PR-Berater des Schweizer Pharmaverbands und des Weltwirtschaftsforums (WEF); der parlamentarische Initiant des Zertifikats, ebenfalls ein PR-Berater der Pharma; der Präsident der Konferenz der kantonalen Gesundheitsdirektoren, zuvor Konzernanwalt beim Pharmaunternehmen Roche; sowie diverse “Experten”, die im Beirat des Pfizer-Forschungspreises sitzen oder den Pfizer-Preis erhalten hatten (siehe Anhang).
Eine gründliche Aufarbeitung dieser Vorgänge wäre wichtig, erscheint aber derzeit schwierig, da die Schweiz über kein Verfassungsgericht verfügt und Regierung, Parlament und Medien alle aktiv an dieser Tragödie mitwirkten, sodass etwa auch eine Parlamentarische Untersuchungskommission (PUK) wie schon bei der Fichen-Affäre wenig Aussicht auf Erfolg hat. Eine aufklärende Rolle könnten möglicherweise gewisse Professoren, unabhängige Journalisten oder Anwälte spielen.
Innerhalb dieses dunklen Kapitels positiv hervorzuheben sind drei Aspekte: Erstens, ein Komitee von über 300 Juristen, Anwälten und Rechtsprofessoren hat sich gegen die Diskriminierung “Ungeimpfter” ausgesprochen und diese als verfassungswidrig kritisiert; zweitens, auch unter Ärzten und Polizisten entstanden Verbände, die sich für Grundrechte einsetzten; drittens, die Schweiz hat als wohl einziges Land der Welt einen Antikörpernachweis für den Genesenenstatus akzeptiert, was medizinisch rational war, aber womöglich ein rein wahltaktisches Ziel verfolgte.
Sowohl international als auch in der Schweiz gibt es Anzeichen, dass das gescheiterte “Covid-QR-Zertifikat” sowie möglicherweise das Contact-Tracing-System (das von Apple und Google in drei Milliarden Mobiltelefone integriert wurde) als Vorläufer für ein digitales Identitäts- und Bezahlsystem dienen soll, das zu einem späteren Zeitpunkt in ein “Sozialkredit-System” nach chinesischem Vorbild erweitert werden könnte. Auch eine medizinisch klar kontraindizierte allgemeine Impfpflicht, wie in einigen Nachbarländern eingeführt, steht weiterhin im Raum.
Impfung und Impfschäden
Die Corona-Impfung hat eine positive und eine negative Seite.
Auf der positiven Seite kann zunächst festgehalten werden, dass die Corona-Impfung die Corona-Hospitalisierungen und Todesfälle bei Schweizer Senioren und Risikogruppen im letzten Jahr stark reduziert hat: die Auswirkungen der Frühlingswelle (Alpha), der Sommerwelle (Delta) und der ersten Winterwelle (nochmals Delta) wurden deutlich gedämpft, wobei für die Winterwelle bereits eine dritte Impfung erforderlich war, da der hohe Impfschutz nur circa 6 Monate hielt. Im Dezember 2021 übernahm dann Omikron, dessen Letalität ohnehin etwa 90% geringer ist.
Insgesamt darf man davon ausgehen, dass die Corona-Impfung in der Schweiz im letzten Jahr bis zu 20’000 Corona-Todesfälle vermieden hat, was etwa 30% der normalen Schweizer Jahressterblichkeit entspricht (ca. 70’000 Todesfälle).
Diesem Erfolg steht indes auch eine erhebliche Anzahl an schweren und tödlichen Corona-Impfnebenwirkungen gegenüber, die Menschen jeden Alters betreffen können und die tatsächlich alle bisherigen Impfnebenwirkungen bei weitem übertroffen haben.
Die Schweizer Heilmittelbehörde Swissmedic hat bis Anfang Februar etwa 12’000 Meldungen zu Covid-Impfnebenwirkungen erhalten, davon rund 4’700 schwerwiegende Nebenwirkungen (mittleres Alter 54 Jahre) und knapp 200 Todesfälle (mittleres Alter 79 Jahre). Internationale Studien kamen zum Ergebnis, dass etwa 80% der gemeldeten Todesfälle und schweren Reaktionen plausibel durch die Covid-Impfstoffe verursacht wurden, aber nur etwa 5% bis 10% der Reaktionen gemeldet werden.
Für die Schweiz ist damit aktuell von knapp 40’000 schwerwiegenden Impfreaktionen und rund 1600 impfbedingten Todesfällen auszugehen. Diese Zahlen passen tatsächlich perfekt zur beobachteten Non-Covid-Übersterblichkeit während der Impfkampagne und insbesondere während der Booster-Kampagne (siehe Grafik unten). Eine ähnliche Non-Covid-Übersterblichkeit parallel zu den Impfrunden wurde in vielen anderen Ländern beobachtet, darunter in Deutschland, England und auch Neuseeland, sowohl bei Senioren als auch bei jungen (insb. männlichen) Personen.
Covid-Impfstoffe schädigen und töten insbesondere durch eine allgemeine Schwächung (bei den ältesten Menschen), durch kardiovaskuläre Reaktionen wie Hirnschläge, Herzinfarkte, Embolien und Herzentzündungen bzw. Herzstillstände, durch temporäre Immunsuppression, sowie durch allergische und neurologische Reaktionen (siehe Übersicht).
Studien haben gezeigt, dass insbesondere bei gesunden Personen unter 40 Jahren die Impfung eher gefährlicher ist als das Coronavirus, zumal die Impfung eine Corona-Infektion und auch potentielles Long Covid bekanntlich ohnehin nicht verhindern kann.
Auch bei Schweizer Profisportlern, Politikern sowie Kindern und Jugendlichen wurde bereits öffentlich über schwere und tödliche Covid-Impfreaktionen berichtet, darunter:
- Der Lausanner Fußballspieler Michael Perrier musste nach einen Herzstillstand und mehrtägigem Koma seine Karriere beenden.
- Die 26-jährige Schweizer Olympia-Sprinterin Sarah Atcho erlitt eine Herzbeutel-Entzündung, nachdem sie trotz Genesung unnötigerweise geimpft und sogar noch geboostert wurde. Auf Twitter schrieb Atcho, sie erhalte “mehr und mehr Meldungen von jungen Leuten, die in der gleichen Situation sind wie ich.”
- Die 31-jährige Schweizer Marathon-Rekordhalterin Fabienne Schlumpf erlitt eine Herzmuskelentzündung nach Impfung und Booster und muss pausieren.
- Impf-Herzschäden sind bei jungen Männern zehnmal häufiger als bei Frauen, weshalb von einer erheblichen Dunkelziffer bei Schweizer Athleten auszugehen ist. Weltweit starben bereits über 400 Athleten im Zusammenhang mit der Covid-Impfung.
- Skistar Lara Gut klagte nach der Impfung während Wochen über Atemprobleme und Leistungsschwäche und infizierte sich dann dennoch mit Corona.
- Tennisstar Belinda Bencic wurde zur Impfung gedrängt, infizierte sich einen Monat später trotzdem mit Corona und klagt seither über Long-Covid-Atemprobleme.
- Der Aargauer Kantonsrat Martin Wernli erlitt durch die Covid-Impfung eine schwere allergische Reaktion und musste seine Politiker-Karriere beenden.
- Der 58-jährige Innerschweizer Politiker Renato Gerig starb im Februar 2022 während einer Gemeinderatssitzung an einem Herzstillstand. Ein Zusammenhang mit der Covid-Impfung ist möglich und plausibel, aber nicht belegt.
- Der Stadtpräsident von Lugano, Marco Borradori (62), starb im August beim Joggen an einem Herzstillstand. Der Co-Direktor des Zürcher Triemli-Spitals, Andreas Zollinger (64), starb im September “überraschend zuhause”. Eine Impfreaktion ist möglich, aber nicht belegt.
- Ein junge Walliser Lehrerin starb an einer impfbedingten Herzentzündung; zwei 17-Jährige angehende Krankenschwestern in St. Gallen starben vermutlich impfbedingt durch eine Hirnblutung bzw. durch eine neurologische Reaktion; und ein Schweizer Schulkind starb durch eine anaphylaktische (allergische) Reaktion (mehr zu diesen Fällen).
Auf der empfehlenswerten Website Covid-Impfnebenwirkungen Schweiz sind zahlreiche weitere Impfschäden und Todesfälle bei jung und alt dokumentiert: Kreislaufkollaps, Herzschäden, Hirnschläge, Autoimmun-Erkrankungen, plötzlicher Hörsturz oder Sehverlust, neurologische Störungen, Gürtelrosen und Nesselfieber, “morgens geboostert, abends tot”, “32 Jahre, Lungenembolie, tot”, Booster-Todesfälle in Altersheimen, und so fort.
Insgesamt ist davon auszugehen, dass die von Behörden und Medien aggressiv propagierte Corona-Impfung in der Schweiz bei jungen und gesunden Erwachsenen unter 40 Jahren sowie bei gesunden Kindern mehr Gesundheitsschäden und Todesfälle verursacht hat und noch verursachen wird, als das Coronavirus selbst, zumal die Corona-Impfung eine Corona-Infektion und mögliches Long Covid ohnehin nicht verhindern kann.
Statt einer beispiellosen Diffamierungs- und Druckkampagne gegen Ungeimpfte – selbst gegen junge Erwachsene und Studenten mit minimalem Corona-Risiko – hätte sich eine rationale und ethische Impfkampagne von Anfang an auf ein Angebot an Senioren, Risikogruppen und weitere Interessierte beschränken müssen.
Medien und Propaganda
Wer sich zum Thema Corona auf die klassischen Schweizer Medien verließ, der landete einmal mehr in der Propaganda-Waschtrommel und wurde beinahe täglich mit Falsch-Information eingeseift, sei es zur Gefährlichkeit des Virus, zur Sinnhaftigkeit der “Maßnahmen”, oder zur Wirksamkeit und Sicherheit der Impfstoffe (siehe “Corona-Fakes in Schweizer Medien”).
Durch die geleakten Aussagen und E-Mails von Ringier-CEO Marc Walder erhielt die Schweizer Öffentlichkeit erstmals einen Einblick in die Medien-Maschinerie und sah, wie sich hinter den Kulissen Regierung und Medienchefs abstimmten, wie sich die Medienchefs untereinander koordinierten, und wie diese Positionen sodann in den Redaktionen von oben nach unten durchgesetzt wurden. Nebenbei: Der Wikipedia-Eintrag zu Ringier-CEO Marc Walder wurde zu 70% vom Benutzer “Ringier AG” verfasst, wie eine Analyse mit WikiWho zeigt.
Viele Corona-Journalisten haben den Bezug zur Realität weitgehend verloren. Das prägnanteste und tragischste Beispiel dürfte der Datenchef von Tamedia sein: zwei Jahre falsche Horrorprognosen; Long-Covid-Dauerpanik ohne seriöse Datengrundlage; haarsträubende Impfpropaganda, die in der Empfehlung zur Off-Label-Impfung von Kleinkindern im Ausland und der Beschimpfung vorsichtiger Ärzte gipfelte und nahtlos ins Leugnen schwerer Impfschäden überging; sowie Märchengeschichten zu einem angeblich natürlichen Ursprung des Virus oder der Wirksamkeit von Masken.
Auch die sogenannte wissenschaftliche Corona-Taskforce lag mit fast allen ihrer Einschätzungen und Prognosen falsch und hatte keinen positiven Einfluss auf das Pandemie-Management. So ging etwa der Schweizer Lockdown Ende Januar 2021, von internationalen Beobachtern mitunter als der “dümmste Lockdown der Pandemie” bezeichnet, auf eine Fehlprognose der Taskforce zurück.
Die Schweizer Wähler haben sich zuletzt in einem Referendum gegen zusätzliche staatliche Förderung der Medienverlage ausgesprochen, aber die essentielle Frage, wie ein unabhängiges und kritisches Mediensystem erhalten bzw. wiederhergestellt werden kann, bleibt offen.
Der österreichische ehemalige Standard-Journalist Ortwin Rosner argumentierte vor kurzem in einer Rede, das derzeitige Mediensystem sei “nicht mehr reformierbar”: man müsse es “absterben lassen und eine neue Medienlandschaft aufbauen, die der Wahrheit verpflichtet ist und nicht der Lüge, die für alle Menschen da ist und nicht bloß für die Mächtigen.”
Kritisch und unabhängig über Corona haben in der Schweiz insbesondere Medien wie der Gesundheitstipp, der Infosperber, die Ostschweiz, sowie teilweise das Fachportal Medside, die NZZ, die Weltwoche, und Inside Paradeplatz berichtet. Hinzu kamen neue kritische Portale und Formate wie etwa Corona-Transition oder StrickerTV. Erwartbar konformistisch waren indes die Republik und die WOZ (siehe den Medien-Navigator).
Ausblick
Die weitere Entwicklung von Corona ist tatsächlich noch offen. Insbesondere stellt sich die Frage, ob sich milde Omikron-Varianten oder aber virulentere Delta-Varianten durchsetzen werden, oder ob sie sich abwechseln werden (wie bei Influenza A und B), und wie gut die verfügbaren Impfstoffe dagegen wirken werden. Auch die Zweckentfremdung des gescheiterten “Covid-Zerifikats” oder eine allgemeine Impfpflicht bleiben reale Szenarien. Es ist zu hoffen, dass die Schweiz auf zukünftige Herausforderungen wieder etwas rationaler, umsichtiger und selbstbewusster reagieren wird.
Sie haben gelesen: Schweiz: Die Corona-Bilanz.
Eine Analyse von Swiss Policy Research.
Anhang: Grafiken und Videos
Anzeigen
A) Non-Covid-Übersterblichkeit parallel zu Booster-Impfungen
Parallel zur Booster-Kampagne (schwarz) nahm die Übersterblichkeit bei Senioren (rot) und danach bei U65 (orange) zu; Corona (violett) erklärt nur etwa ein Drittel dieser Todesfälle.

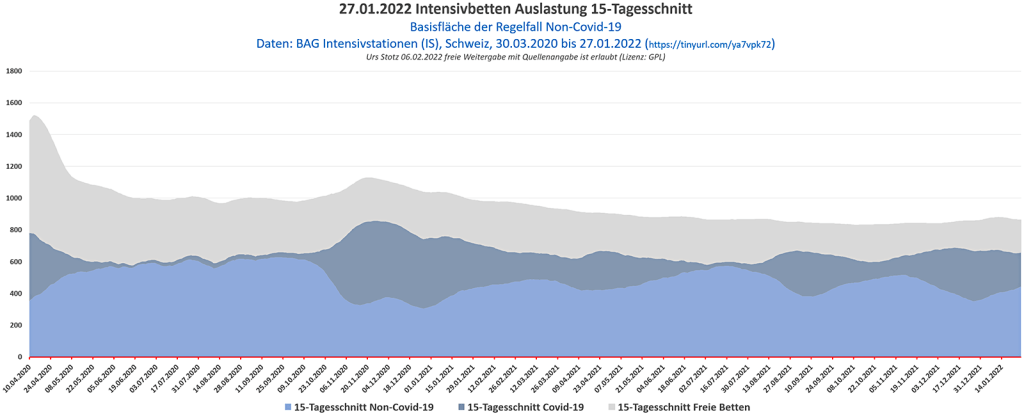
B) Intensivbetten-Belegung
Grundauslastung (hellblau), Corona (dunkelblau), unbelegt (grau).
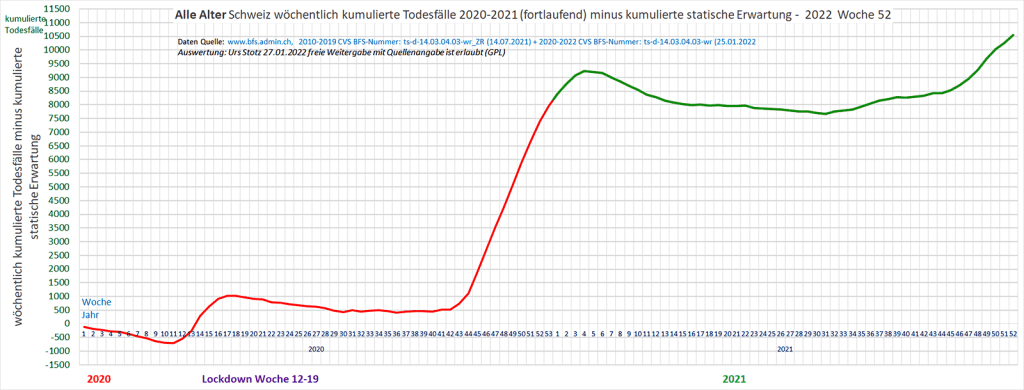
C) Kumulierte Übersterblichkeit 2020-2021
Die kumulierte Übersterblichkeit seit Januar 2020 lag Ende 2021 bei ca. 10’500 Personen.
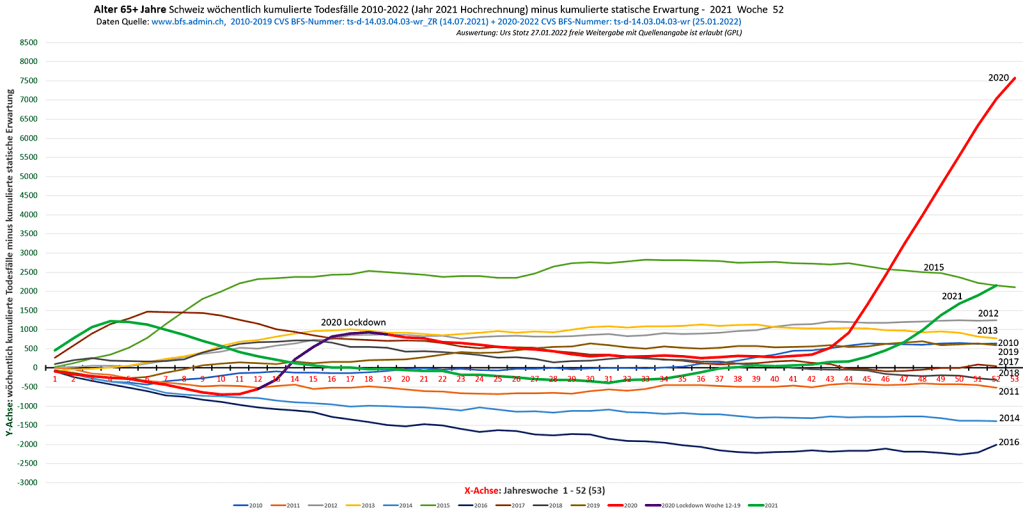
D) Übersterblichkeit 65+, 2010-2021
Das Jahr 2020 erreichte eine Mortalität wie zuletzt in den Jahren 2000 und 2003.
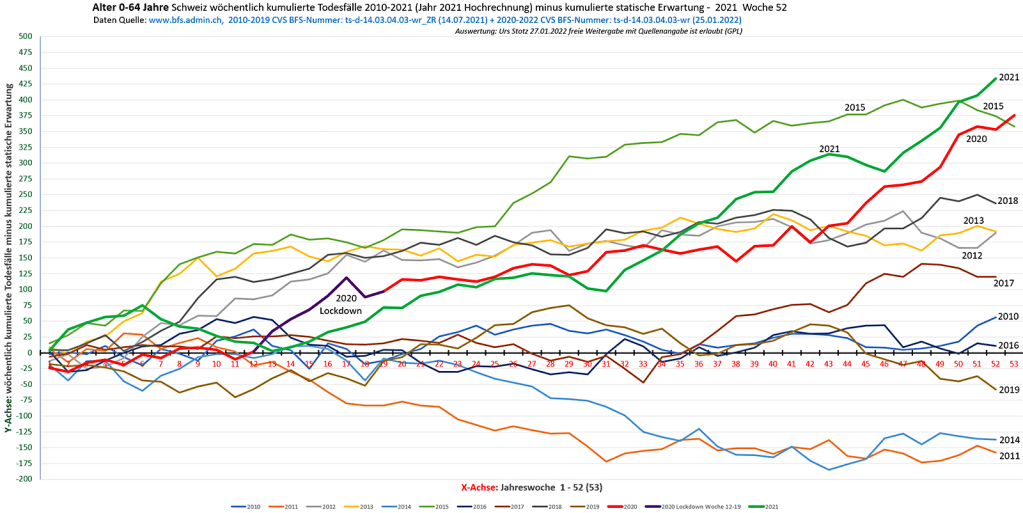
E) Übersterblichkeit 0-64, 2010-2021
Für U65 war 2021 ein schlechtes Jahr, was an Delta und ev. der Impfung liegen könnte.
F) Lockdown, Lockerungen, Impfpässe ohne Einfluss
Die Schweizer Lockdowns im Winter 2020/21, Lockerungen im Frühjahr 2021, und Impfpässe seit Herbst 2021, hatten keinen Einfluss auf den Verlauf der Pandemie.

G) Schweiz: Interventionen und Infektionen
Das phänomenale Scheitern von Masken und “Covid-Zertifikaten”.

H) Geimpfte und Ungeimpfte: Gleiche Viruslast
Geimpfte und Ungeimpfte sind gleich ansteckend. (Studie)

J) TV-Experte und Beirat des Pfizer-Forschungspreises
TV-Infektiologe Huldrych Günthard sitzt im Beirat des Pifzer-Forschungspreises; der Chef der Eidgenössischen Impfkommission, Christoph Berger, sowie mindestens ein (ehemaliges) Mitglied der Taskforce sind Pfizer-Preisträger.
K) Schließung der Walliserkanne
Polizeiliche Schließung des Restaurants Walliserkanne in Zermatt wegen wiederholter Nicht-Umsetzung der Zertifikate-Vorschriften (November 2021). Auch gegen kritische Ärzte kam es wiederholt zu behördlichen Maßnahmen und sogar zu Polizeiübergriffen.

L) Robert F. Kennedy Junior in Bern
Robert F. Kennedy Jr., der Neffe des ehemaligen US-Präsidenten, besuchte am 12. November 2021 Bern und empfahl den Schweizern, “Impfpässe” abzulehnen. Mehr zu seinem Besuch.